Ear infections are the bane of modern parenthood. Yet, they are poorly understood and often over-treated. The United States spends $4 billion a year on ear infections. I do not think this needs to be the case. Once I began practicing integrative medicine and incorporating nutritional recommendations into my daily pediatric practice, I saw recurrent ear infections melting away.
This phenomenon was corroborated by mothers of kids with autism I was seeing in my practice. These kids were eating a very clean diet and not only were they free of recurrent ear infections, but they were also staying healthy when the rest of the household had the stomach bug or the flu.
So what was I witnessing? I am not 100% sure, but let me share with you my best-educated summary.
This is by no means a comprehensive analysis of the recurrent cycle of ear infections many kids face. It simply explains how I’ve come to understand and treat ear infections in my practice. First, let’s start with the causes.
Four Basic Things Contribute to Ear Infections:
- Viruses
- Bacteria
- Environmental allergies and food allergies/sensitivities
- Eustachian tube dysfunction
Viruses are not living organisms, rather, they are DNA or RNA inside a coated protein. They spread rapidly by invading our own cells and forcing them to make copies of the virus, destroying our cells in the process. For example, the Rhinovirus causes the “common cold.” Antibiotics do not kill viruses. It is up to our own body’s immune system to take care of viral infections.
Bacteria are uni-cellular living microorganisms. They have DNA and RNA within their cell wall. A simple infection caused by bacteria is often localized to a certain area, such as the middle ear or sinus cavities. Some bacteria are beneficial, especially the so-called “friendly flora” in the gut. Fun factoid: we have more bacteria in our guts than we have cells in our bodyJ
Environmental allergies and food allergies/sensitivities can cause a great deal of inflammation. Both can lead to inflammation of the tissues lining the sinus cavities and the nose, and all of this further contributes to runny noses, post-nasal drip, cough, watery itchy eyes, and sometimes itchy skin.
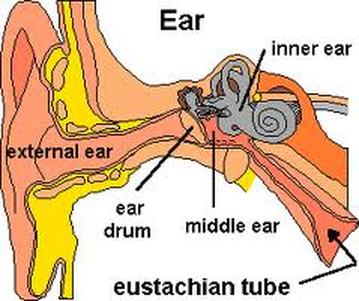
Eustachian tube dysfunction is medical speak for when that beautifully designed tube that runs from the middle ear to the back of the nose (and throat) is not functioning properly. This tube allows fluid to drain into and out of the middle ear. When it is swollen, it essentially becomes a dam and allows a little pool of fluid to be held hostage in the middle ear, creating the perfect circumstances for bacteria to grow. This issue can be a structural problem or an inflammatory one. Both of which do not allow the tube to function in the way it is supposed to.
How Infection Sets In
The tissues of the body (like the nasal mucosa and the sinus cavities also have the ability to resorb (or absorb) fluid that has collected in the middle ear.
However, if the tissues are swollen, as they are with allergies or a bad cold, the tissue’s ability to resorb fluid is drastically reduced. If the nose is swollen and filled with mucous, there is nowhere for this fluid to go. When this fluid is allowed to lay dormant in the middle ear, it becomes a breeding ground for bacteria and viruses.
If you think about the setup, a clogged middle ear is similar to a warm bathtub that is allowed to sit un-drained for several days. It quickly becomes a cesspool teaming with bacteria!
Why So Many Kids Have Chronic Runny Noses: Is It Really Daycare?
So this begs the question, why do so many kids have so much mucous, inflammation, and so many runny noses? If you ask ten different pediatricians, many of them will likely blame daycare centers. And yes, I do agree this is a big part of the reason. However, I think poor nutrition (in particular a high intake of dairy and refined sugars) plays an even bigger role and is more easily addressed (at least theoretically).
In my experience, if a child is eating optimal nutrition, and following some other very basic guidelines for enhancing their immune system, they can still go to daycare and ward off the many offending viruses and bacteria that daycares can often harbor.
How an ear infection starts
What this looks like in real time with your child:
- Children are exposed to a virus that causes the common cold or allergy season hits. The body begins to produce excess mucous and it is secreted into the nasal passages and sinus tissues.
- The child may have a brief period of time where fluid pools in the middle ear.
- A child with a healthy immune system will be able to clear the fluid, including the viral infection within several days, even if a small amount of bacteria has begun to grow.
- A child whose system is inflamed and stressed will have a lingering runny nose, congestion and cough. This is when the fluid pools in the middle ear and sets up the perfect conditions for bacteria to proliferate.
** And this is what we call an ear infection.
Upwards of 65% of ear infections will heal on their own, without the aid of an antibiotic. It is safe to watch and wait in certain scenarios depending upon the age of the child, their overall health status, the structure of their ear anatomy, and their past medical history. The American Academy of Pediatrics (AAP) calls this the watch and wait approach. Here is the full AAP guidelines.
The good news is, many children will out-grow ear infections.
When babies are born, their Eustachian tubes are, for all practical purposes horizontal between the ear and the nose. As the baby grows, this begins to take on a more vertical angle. By the time the baby is two years old, the Eustachian tube should be at its more adult-like vertical angle. This is why adults have fewer ear infections than children; anatomy is on our side.
References:
- Bahna SI, Myer CM. food allergy for the pediatrician. Int Pediatr 1988;3:245-9.
- Bock SA, May CD. Adverse reactions to food caused by sensitivity. In: Middleton EM, Reed CE, Ellis EF, eds. Allergy principles and practice. St. Louis, MO: CV Mosby, 1988;1415-27.
- Kettelhut BV, Metcalfe DD, Adverse reactions to foods. In: Middleton EM, Reed CE, Ellis EF, eds. Allergy principles and practices, St Louis, MO: CV Mosby, 1988:1481-502.
- Nsouli et al. The Role of Food Allergy in Serous Otitis Media. Annals of Allergy 1994;73(3):215-219.






